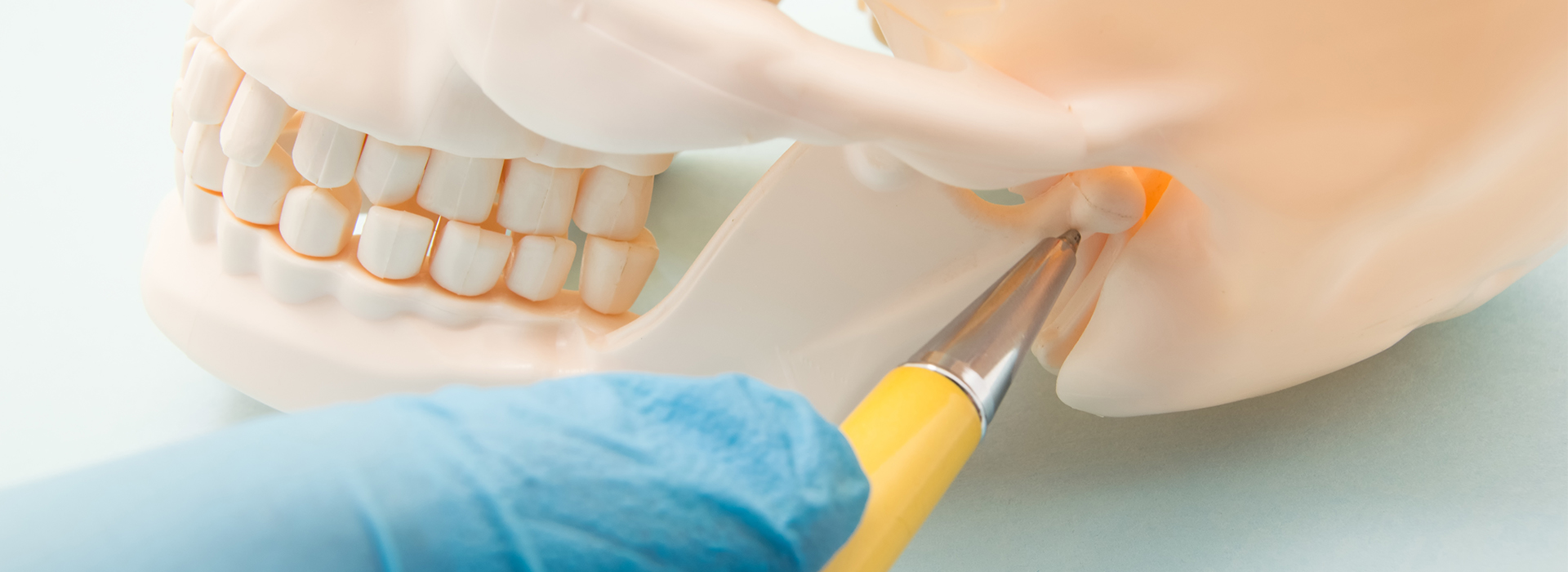
Temporomandibular joint (TMJ) disorders affect how the jaw moves and how comfortable everyday activities like chewing, speaking, and yawning feel. National estimates show millions of people experience some form of TMJ-related pain or dysfunction during their lives, and the condition ranges from short-lived jaw soreness to chronic, life-disrupting problems. This page explains what the TMJ does, common triggers for trouble, how clinicians evaluate the condition, and the treatment options patients can expect.
The temporomandibular joint is actually a paired complex on each side of the face that links the lower jaw (mandible) to the temporal bones of the skull. Each joint contains a small, fibrous disc that cushions motion between the rounded condyle of the lower jaw and the socket in the skull. Surrounding muscles, ligaments and tendons coordinate to allow hinge movements as well as forward, backward and side-to-side sliding actions, making the TMJ one of the most mechanically versatile joints in the body.
Because the TMJ must perform a wide variety of movements while bearing the forces generated by biting and chewing, it can be vulnerable to wear, strain and injury. Even subtle changes in how the teeth meet, prolonged muscle tension, or an acute injury can alter coordinated joint mechanics and lead to pain, restricted motion, or abnormal noises such as clicking or popping.
Understanding this interplay between anatomy and function helps patients and clinicians focus on practical strategies to protect the joint — from modifying habits that overload the system to targeting underlying mechanical or inflammatory problems that compromise normal movement.
TMJ disorders arise from a mix of mechanical, biological and behavioral factors. Teeth grinding (bruxism) or clenching is a common contributor because it elevates the sustained force across the jaw muscles and joint surfaces. Trauma to the jaw or head, such as a blow or sudden forceful opening, can also displace the joint disc or damage soft tissues and cartilage.
Degenerative conditions like osteoarthritis or inflammatory diseases such as rheumatoid arthritis may progressively alter joint structure and function, increasing vulnerability to pain and stiffness. Hormonal and genetic influences can also play a role in susceptibility, which helps explain why TMJ problems are more common in some people than others.
Stress and muscle tension are important behavioral contributors. Chronic stress often manifests as tightened jaw and neck muscles, and over time that imbalance can create myofascial pain or disrupt the coordinated actions of the TMJ complex. Identifying and addressing these contributing factors is a key first step in a successful treatment plan.
While jaw pain is the most obvious sign of a TMJ issue, symptoms frequently extend beyond the joint itself. Many patients report ear-related complaints — fullness, aching, or ringing (tinnitus) — without an underlying ear infection. Headaches that start near the temples, facial pain, or a sense of pressure around the cheekbones and eyes are also common and can be mistaken for other conditions.
Mechanical symptoms are another hallmark: clicking, popping or grinding sounds when opening or closing the mouth; episodes of the jaw catching or locking in an open or closed position; and a feeling that the bite has shifted or does not close as smoothly as it once did. In some cases, range-of-motion is reduced and patients struggle with wide opening or chewing tougher foods.
Because TMJ-related symptoms can overlap with dental, neurological and ear-nose-throat conditions, a careful clinical evaluation is important to separate TMJ disorders from other causes and to design treatment that targets the right problem areas.
If symptoms are intermittent and mild, many people find relief with behavioral changes and self-care. When pain or dysfunction persists or interferes with daily activities, seeking a professional assessment is the prudent next step.
A thorough evaluation begins with a detailed history and clinical exam. The clinician will ask about the onset and quality of symptoms, patterns of pain, and habits such as clenching, gum chewing or sleep bruxism. Palpation of the jaw muscles and joint, observation of jaw movements, and assessment of how the teeth fit together help build a picture of how the joint is functioning.
Diagnostic imaging is used selectively to refine the diagnosis. Panoramic X-rays, cone-beam CT scans, and MRI can reveal structural changes to the bone, joint surfaces, or the position of the joint disc. MRI is particularly helpful when internal derangement — such as disc displacement — is suspected because it visualizes soft tissues and disc relationships.
Because TMJ disorders often reflect a combination of muscular, dental, and joint issues, many clinicians collaborate with or refer to physical therapists, oral surgeons, or medical specialists when specialized care is needed. Working within a multidisciplinary framework improves diagnostic accuracy and helps match treatments to the root causes identified during evaluation.
Most treatment programs begin conservatively and escalate only as necessary. Early approaches emphasize symptom relief and restoring comfortable function: short-term soft diet, avoiding wide yawning and gum chewing, applying heat or ice as advised, and practicing guided jaw relaxation and stretching exercises. Patients are often taught techniques to reduce clenching and manage stress-related muscle tension.
Oral appliances, such as custom night guards or stabilization splints, can be very effective for reducing clenching forces and protecting the teeth and joints from excessive wear. These devices are tailored to the patient’s bite and may be used in combination with physical therapy to re-balance muscle activity and improve coordinated movement.
For persistent inflammation or structural problems, other options may be considered. Injectable therapies can reduce local inflammation and break painful muscle spasm patterns in some cases. Occlusal adjustments, orthodontic intervention, or prosthodontic treatment are sometimes necessary when tooth alignment or bite relationships contribute directly to joint stress. Surgery is reserved for a small subset of patients with severe internal derangement or degenerative changes that have not responded to conservative care.
Throughout treatment, the goal is to restore comfortable, efficient jaw function while minimizing pain and preventing recurrence. Individualized plans — informed by a careful diagnosis and scaled to the severity of the condition — typically deliver the best long-term outcomes.
If you suspect you have a TMJ disorder or your jaw symptoms are becoming more frequent or severe, our team can evaluate your condition and outline practical options. Comprehensive Family Dentistry helps patients navigate the diagnostic process and offers conservative, evidence-informed care to preserve jaw health and comfort. Contact us to learn more about available treatments and to discuss what approach is best for your situation.

The temporomandibular joint (TMJ) links the lower jaw to the temporal bones of the skull and enables the hinge and sliding movements required for chewing, speaking and yawning. Each side of the jaw contains a small fibrous disc and a network of muscles and ligaments that coordinate those movements. When those tissues are injured, inflamed, or functioning abnormally, the result is a TMJ disorder that can cause pain and limited motion.
TMJ disorders exist on a spectrum from brief soreness after unusual use to chronic conditions that interfere with daily activities. Symptoms can fluctuate over time and may be influenced by muscular tension, dental factors, trauma, or degenerative joint disease. Recognizing the joint's anatomy and mechanics helps patients and clinicians choose treatments that protect function and reduce pain.
TMJ disorders are usually multifactorial, meaning several issues contribute to dysfunction rather than a single identifiable cause. Common contributors include teeth grinding (bruxism), clenching, direct trauma to the jaw, and degenerative changes such as osteoarthritis. Structural problems with the joint disc or bone can develop after an injury or gradually with wear and tear.
Behavioral and environmental factors like chronic stress, poor posture, and repetitive chewing habits can perpetuate muscle tension and joint overload. Sleep bruxism is a frequent contributor because it applies sustained forces to the joint during hours of rest. Identifying and addressing these modifiable behaviors is a key component of effective treatment planning.
Many patients with TMJ disorders report non-jaw symptoms such as ear fullness, tinnitus, or a feeling of ear pressure without an actual ear infection. Headaches that begin near the temples, facial aching, and pain radiating to the neck and shoulders are common and can mimic other conditions. Noisy joint sounds—clicking, popping, or crepitus—often accompany these complaints and may indicate altered disc motion or joint surface changes.
Mechanical problems like jaw locking, catching, or a changed bite are also typical and can limit how widely a patient can open their mouth or how comfortably they chew. Some people notice that routine activities such as yawning, singing, or eating hard foods provoke or worsen their symptoms. When symptoms interfere with sleep, speech, or eating, professional assessment is recommended to prevent deterioration.
Diagnosing a TMJ disorder starts with a detailed medical and dental history and a focused clinical examination of jaw motion, muscle tenderness, and how the teeth come together. Palpation of the muscles and joints, observation of opening and closing patterns, and assessment of range of motion build the initial diagnostic picture. The clinician will also ask about habits such as clenching, gum chewing, and sleep grinding to identify behavioral contributors.
When indicated, imaging studies refine the diagnosis; panoramic x-rays and cone-beam CT show bony anatomy while MRI visualizes soft tissues and disc position. MRI is particularly useful for suspected internal derangement because it reveals the relationship between the disc and joint surfaces. Because TMJ disorders can involve muscular, dental, and joint components, collaboration with physical therapists or oral surgeons may be recommended for comprehensive care.
Conservative care is the first-line approach for most TMJ problems and focuses on pain relief, reducing joint load, and restoring comfortable motion. Common initial measures include a short-term soft diet, avoiding wide mouth opening or gum chewing, and using heat or cold as directed to control muscle spasm and inflammation. Guided jaw relaxation and gentle stretching exercises help re-establish coordinated muscle function and can be taught in the dental office or by a physical therapist.
Physical therapy, including manual techniques and therapeutic exercise, is often combined with home strategies to address muscle imbalance and posture-related contributors. Short courses of anti-inflammatory medications or muscle relaxants may be used under a clinician's guidance to control pain and improve participation in therapy. When conservative measures are insufficient, additional interventions such as occlusal appliances or injectable therapies may be considered based on the specific diagnosis.
Custom oral appliances are commonly recommended when clenching or sleep bruxism is a major contributor to joint symptoms or when protection of teeth and restorations is needed. A stabilization splint or night guard redistributes bite forces, reduces muscle hyperactivity, and can diminish joint loading during sleep. These devices are fabricated from impressions or digital scans to fit the individual's bite and are adjustable to optimize comfort and function.
Patients typically wear them at night initially while the clinician monitors symptom response and makes refinements as necessary. Oral appliances can also be useful as part of a broader program that includes physical therapy, stress management, and behavior modification. Long-term appliance use may require periodic reassessment to ensure it continues to protect the teeth and support healthy jaw mechanics.
Dental factors such as missing teeth, poorly fitted restorations, or significant changes in bite relationships can alter how forces are distributed across the TMJ. When the occlusion forces the jaw into abnormal positions, muscles and joints may compensate, leading to pain and dysfunction over time. Restorative or prosthetic treatment that changes bite relationships may require careful planning to minimize added joint stress.
In some cases, orthodontics, occlusal adjustment, or prosthodontic rehabilitation are part of a comprehensive plan when dental alignment is a clear driver of joint problems. These interventions are individualized and are typically considered only after conservative measures and thorough diagnostics clarify the role of dental factors. Treatments are coordinated with the patient’s functional needs to balance joint health with long-term dental stability.
Surgical intervention for TMJ disorders is reserved for a small subset of patients who have persistent, disabling symptoms or clear structural abnormalities that do not respond to conservative care. Indications may include severe internal derangement with recurrent locking, advanced degenerative joint disease, or tumors and ankylosis affecting joint motion. Because surgical procedures carry risks, they are undertaken only after careful diagnostic work-up and discussion of expected benefits and limitations.
Whenever surgery is considered, second opinions and multidisciplinary review improve decision-making and outcomes. Common surgical options range from minimally invasive arthroscopy to open joint reconstruction, each with different indications and recovery timelines. Postoperative rehabilitation is critical to restoring function, and long-term follow-up helps identify and manage complications or recurrences.
Between visits, patients can take several practical steps to reduce TMJ symptoms and support recovery. Adopting a soft diet, avoiding hard or chewy foods, and minimizing wide mouth opening reduces mechanical stress on the joint and surrounding muscles. Applying moist heat or ice during acute flare-ups, practicing gentle jaw stretches, and learning relaxation techniques help control pain and decrease muscle tension.
Good posture, especially when using phones or computers, further reduces strain on neck and jaw muscles. Consistent sleep habits and addressing nighttime grinding—through behavior strategies or an oral appliance—can significantly improve symptoms for many patients. If home measures do not lead to steady improvement or if symptoms worsen, patients should schedule a professional evaluation to avoid progression.
Comprehensive Family Dentistry in Miami Lakes offers an evidence-informed approach to diagnosing and managing TMJ disorders, emphasizing conservative care and individualized treatment planning. Our team performs detailed clinical evaluations, uses selective imaging when necessary, and coordinates care with physical therapists or specialists when appropriate. The practice’s state-of-the-art office and focus on patient education support predictable, conservative management strategies aimed at restoring comfortable function.
When collaborative care is needed, the office maintains referral pathways to oral surgeons and other medical specialists to ensure all aspects of a patient’s condition are addressed. Follow-up and reassessment are part of the standard protocol to measure progress and adjust the plan as needed for long-term outcomes. Contacting the Miami Lakes office to request an evaluation is appropriate for anyone whose jaw pain or mechanical symptoms persist despite self-care.

Whether you’re ready to schedule your next dental appointment or simply have questions about our services, connecting with our team has never been easier.
Our friendly team is here to assist with appointment scheduling, answer questions about treatments, and address any concerns you may have. You can call or use our convenient online form to get in touch.
Take the first step toward a healthier, more confident smile—contact us today and experience the difference personalized dental care can make.