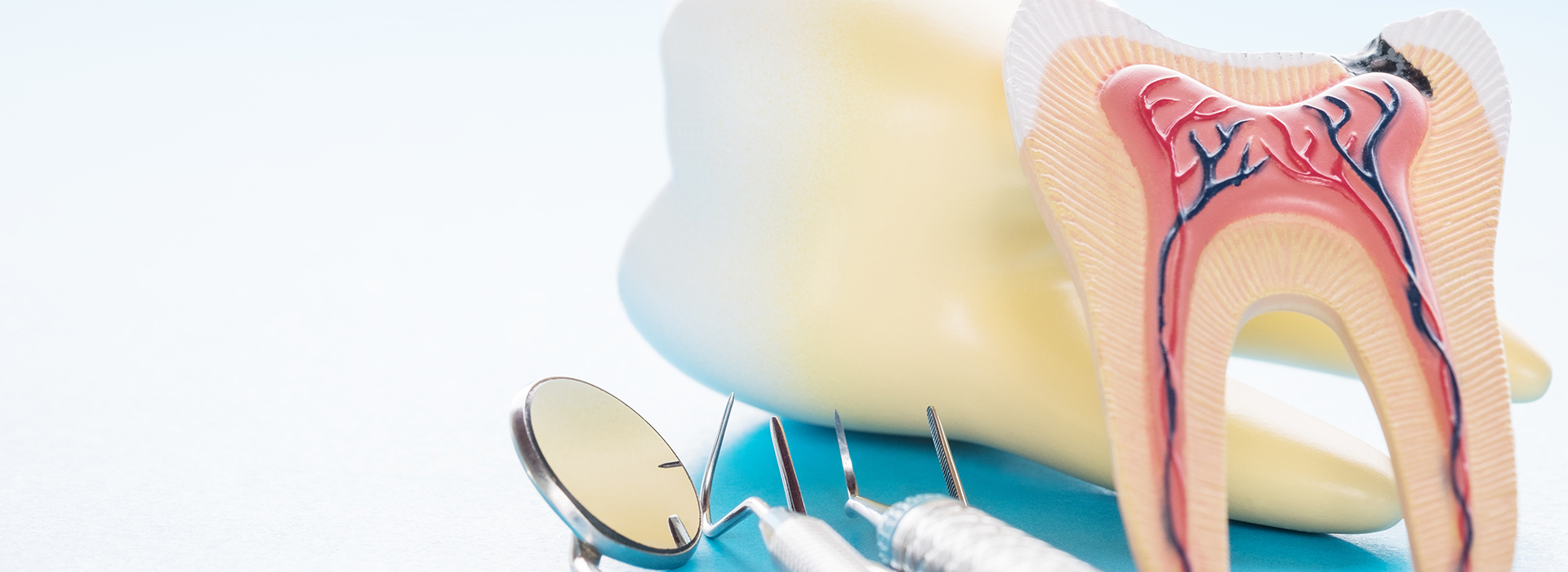
Being told a tooth needs a root canal can sound intimidating, but modern endodontic care is highly predictable and focused on comfort. A root canal procedure removes damaged or infected inner tissues, relieves persistent tooth pain, and helps you keep your natural tooth where possible — often a better long-term option than extraction.
At Comprehensive Family Dentistry, we combine careful attention to comfort with contemporary treatment methods so patients receive precise, minimally invasive care. Our goal is to protect your oral health while keeping you informed and at ease throughout the process.
Root canal therapy targets the dental pulp — the soft tissue inside a tooth that contains nerves and blood vessels — when it becomes inflamed or infected. By removing damaged tissue and sealing the internal spaces, the procedure stops infection from spreading and restores the tooth’s structural stability. With modern materials and techniques, treated teeth can function for many years or even a lifetime.
Clinical success rates for contemporary root canal therapy are high, in large part because of advances in diagnostic imaging, instrumentation, and filling materials. Instead of losing a tooth and altering adjacent teeth with bridges or removable appliances, preserving your natural tooth helps maintain normal bite forces and reduces long-term complications for surrounding teeth and bone.

Every case is unique, and alternatives to root canal therapy may be discussed when appropriate. However, when the internal tissues of a tooth are irreversibly damaged, endodontic treatment is frequently the most conservative way to maintain your smile and oral function.
Understanding why a root canal might be recommended starts with knowing what the dental pulp does and how problems develop. The pulp supports a tooth’s development and senses temperature and pressure. When decay, deep fillings, trauma, or infection compromise that tissue, symptoms often follow — sometimes gradually, sometimes suddenly.
Symptoms can vary widely. Some patients experience sharp, lingering pain with hot or cold, while others notice swelling, a darkening tooth, or discomfort when biting. In other cases, an infected tooth produces little immediate pain but shows changes on X-rays that indicate the need for treatment. A careful clinical exam and radiographic assessment help determine the root cause.
Prompt attention to warning signs improves the odds of a straightforward outcome. The list below outlines common indicators that a tooth may require endodontic therapy, but not every sign means a root canal is required — your dentist will evaluate the whole picture before recommending treatment.
Although not every instance of dental discomfort indicates the need for root canal therapy, some of the warning signs that you might require this procedure include the following:
Pain that persists or wakes you at night is a key signal that internal tooth tissues may be compromised. While many dental issues can cause discomfort, a deep ache that does not subside with routine care often points to pulpal inflammation or infection.
When simple sensations like a hot drink or an ice cube trigger intense or long-lasting discomfort, the nerve supply inside the tooth may be inflamed. This abnormal sensitivity is an important diagnostic clue.
Discomfort from pressure often indicates that the tooth’s internal tissues are compromised or that infection has reached supporting structures. Patients frequently describe a sharp or localized pain with chewing.
A tooth that darkens after trauma or over time can be a sign that the pulp has been injured or has died. Color changes alone don’t mandate treatment, but they often accompany other signs of internal damage.
Structural damage can expose or damage the pulp, allowing bacteria to enter and create infection. Even when a tooth looks intact externally, an internal crack can still affect the pulp and necessitate care.
Gum swelling, tenderness, or a pimple-like bump near the tooth are signs that infection may have spread beyond the root tip. Such findings typically require prompt evaluation and treatment to prevent further complications.
Infection that affects the bone supporting a tooth can cause mobility. Addressing the source of infection through root canal therapy often allows healing and stabilization of the tooth.
Delaying evaluation or treatment when symptoms appear increases the chance that infection will spread and the situation will become more complex. Early intervention can stop decay or infection before it undermines surrounding bone or adjacent teeth, simplifying treatment and improving outcomes.
Radiographs taken during routine exams can reveal issues that aren’t yet painful. Sometimes a tooth will appear stable in the mouth while X-rays show changes at the root tip. Identifying these concerns early allows your dentist to recommend conservative care rather than waiting for an acute problem to develop.
When a root canal is recommended, prompt scheduling and treatment reduce the likelihood of complications such as persistent infection, extensive bone loss, or the need for extraction. Treating the tooth while sufficient structure remains also increases the chance of restoring it with a durable crown or other restoration.
Root canal procedures today are precise, comfortable, and designed to preserve as much natural tooth as possible. Treatment generally begins with local anesthesia to numb the tooth and surrounding tissues. If you have dental anxiety, additional sedation options can be discussed to make the visit more relaxed.
Once anesthetized, the dentist or endodontist creates a small opening to access the pulp chamber and root canals. Specialized instruments are used to gently remove diseased tissue, clean and shape the canal spaces, and disinfect the internal surfaces. The canals are then filled with a biocompatible material to seal them against future infection.
The complexity of the tooth — for example, whether it has one canal or several — and whether there is an active infection influence how many visits are required. Some cases are completed in a single appointment; others may need two visits to ensure complete healing and proper sealing.
After the internal portion of the tooth is treated, the final step is restoring it with a durable filling or crown. This rebuilds strength and function, protecting the treated tooth from fracture and allowing you to chew normally with confidence.
At Comprehensive Family Dentistry, patient comfort and education are key parts of post-treatment care. Following a root canal, it’s common to experience mild soreness for a few days as surrounding tissues heal. Over-the-counter anti-inflammatory medications typically manage this discomfort; we will advise you based on your individual needs.
Immediately after the appointment, expect temporary numbness until the local anesthetic wears off. During this time, avoid chewing on the treated side to prevent accidental injury. If antibiotics are prescribed for a specific infection, take them exactly as directed to support healing.
Oral hygiene remains important after treatment. Continue to brush and floss gently around the treated tooth and the rest of your mouth. Because a tooth that has had a root canal can be more prone to fracture until it is fully restored, timely placement of a crown or permanent restoration is usually recommended.
Initial sensitivity when biting and mild soreness are common and typically resolve within days to a few weeks. If pain intensifies or swelling develops, contact the office for prompt reassessment.
When indicated, antibiotics and pain medications will be prescribed or recommended. Attend any scheduled follow-up visits so your clinician can confirm healing and finalize the restoration.
Until a permanent restoration is in place, avoid hard or sticky foods on the treated side. Once restored with a crown, the tooth will be better protected and should function normally for many years with good home care.
With proper restoration and ongoing oral hygiene, a tooth that has undergone root canal therapy can remain healthy and functional for the long term. Routine dental visits help monitor the restoration and surrounding tissues.
If you notice persistent discomfort, unusual swelling, or any signs of infection after treatment, contact our office so we can evaluate and address your concerns quickly. Timely follow-up ensures the best possible outcome for your treated tooth.

A root canal is a dental procedure that removes diseased or injured pulp, the soft tissue inside a tooth that contains nerves and blood vessels. The goal is to eliminate infection, relieve pain and preserve the natural tooth when possible. Because the pulp does not affect the tooth’s ability to chew once removed, many teeth function normally after treatment.
Modern root canal therapy uses advanced diagnostic imaging, rotary instruments and biocompatible filling materials to clean and seal the internal spaces of the tooth. These improvements have increased clinical success rates and reduced the need for extraction in many cases. Restoring the treated tooth with a durable filling or crown helps protect it from fracture and supports long-term function.
A root canal may be recommended when the pulp is inflamed or infected due to deep decay, a large filling, trauma or a crack that allows bacteria to enter. Symptoms that commonly accompany pulp problems include persistent toothache, heightened sensitivity to hot or cold and pain when biting. Some teeth may darken or show radiographic changes before causing noticeable discomfort.
Not every tooth that hurts requires a root canal, and the final determination depends on a clinical exam and X-rays. Early evaluation increases the chance of a routine treatment and avoids complications such as spread of infection to surrounding bone. Your dentist will consider the tooth’s restorability, overall oral health and alternative treatments before recommending therapy.
A modern root canal appointment begins with local anesthesia to numb the tooth and surrounding tissues, making the procedure comfortable for most patients. The dentist or endodontist then creates a small access opening to reach the pulp chamber and root canals. Specialized files and irrigants gently remove diseased tissue and disinfect the canal system, and canals are shaped to receive a filling material.
The canals are filled with a biocompatible material and sealed to prevent reinfection. Some teeth can be treated in a single visit, while others with active infection or complex anatomy may require two appointments to ensure complete cleaning and sealing. After the internal portion is completed, the tooth is restored with a permanent filling or a crown to rebuild strength and prevent fracture, and Comprehensive Family Dentistry discusses sedation options and restoration timing to match each patient's needs.
Most patients report little or no pain during a root canal because of effective local anesthesia and modern techniques. Discomfort during the appointment is uncommon, and clinicians take steps to maintain patient comfort throughout treatment. If anxiety is a concern, additional sedation options can be discussed to create a more relaxed experience.
Mild soreness or sensitivity for a few days after treatment is normal as surrounding tissues heal, and over-the-counter anti-inflammatory medications usually manage this discomfort. If pain intensifies, swelling develops or symptoms persist beyond a week, contact the office for prompt reassessment. Comprehensive Family Dentistry provides patient education and individualized post-operative instructions to support smooth recovery.
Immediately after a root canal you may have temporary numbness from local anesthesia and should avoid chewing until sensation returns. Most patients resume normal eating within a day or two as tenderness subsides. If the case included an active infection, additional recovery time may be needed and follow-up visits help monitor healing.
Do not chew hard or sticky foods on the treated tooth until it is fully restored to reduce the risk of fracture. If antibiotics are prescribed, take the full course exactly as directed and attend any scheduled follow-up appointments. Call the office if you experience increasing pain, swelling or signs of systemic illness such as fever.
After root canal therapy the tooth usually needs a permanent restoration to restore strength and protect it from fracture. A direct filling may be appropriate for small teeth with adequate remaining structure, while posterior teeth often benefit from a crown for long-term durability. The timing of the final restoration depends on healing, the complexity of the case and whether the tooth needs a temporary filling between visits.
Prompt restoration helps preserve function and reduces the risk of future complications. With proper restoration and routine dental care the treated tooth can remain functional for many years. Regular dental exams and X-rays allow your dentist to monitor the integrity of the restoration and the surrounding bone.
Alternatives to root canal therapy include monitoring the tooth, performing a more conservative vital pulp therapy in specific cases, or extracting the tooth when preservation is not feasible. Vital pulp therapies such as pulpotomy or partial pulpectomy are sometimes appropriate for immature or recently injured teeth. Extraction removes the source of infection but introduces the need to consider replacement options to maintain chewing function and prevent drifting of adjacent teeth.
Your dentist will weigh factors such as the tooth’s restorability, remaining tooth structure and overall oral health when discussing alternatives. Imaging, clinical findings and patient goals guide the recommendation so that treatment aligns with long-term oral function. A thoughtful discussion of risks and benefits helps patients make informed choices about care.
A root canal can fail when bacteria remain in a complex canal system, when a new leak occurs around the restoration or when a previously undetected fracture affects the root. Symptoms of failure may include recurrent pain, swelling or radiographic signs of persistent infection at the root tip. Not all post-treatment symptoms indicate failure, so careful clinical and radiographic evaluation is essential.
If a treated tooth does not heal, options can include nonsurgical retreatment, surgical endodontic procedures such as an apicoectomy, or extraction when retreatment is not predictable. The chosen approach depends on the cause of failure, tooth anatomy and the condition of the existing restoration. Timely assessment and treatment improve the likelihood of saving the tooth when possible.
Children can require endodontic care when deep decay or trauma reaches the pulp of a primary or young permanent tooth. Treatment goals in pediatric cases focus on eliminating infection while preserving tooth function and supporting normal development of the jaw. Techniques differ from adult care and may include pulpotomy, pulpectomy or full root canal therapy depending on tooth maturity.
The dental team uses behavior guidance and, when appropriate, sedation to provide safe and comfortable care for young patients. Follow-up visits ensure healing and allow timely placement of protective restorations to prevent reinfection or fracture. Early detection of decay and prompt treatment reduce the chance that a child will need complex endodontic procedures later.
You can reduce the risk of needing a root canal by practicing consistent oral hygiene, including brushing twice daily with fluoride toothpaste and daily flossing to control decay and gum disease. Regular dental exams and X-rays identify decay and cracks early, allowing conservative treatment before the pulp is affected. Wearing a protective mouthguard during sports and avoiding chewing hard objects also lowers the risk of traumatic injuries that can compromise the pulp.
Maintaining overall health, including controlling conditions like diabetes, supports healing and reduces oral infection risk. Promptly addressing new dental symptoms or visible damage increases the chance for simple repairs instead of endodontic treatment. Routine professional care and early intervention remain the most effective ways to protect your natural teeth long term.

Whether you’re ready to schedule your next dental appointment or simply have questions about our services, connecting with our team has never been easier.
Our friendly team is here to assist with appointment scheduling, answer questions about treatments, and address any concerns you may have. You can call or use our convenient online form to get in touch.
Take the first step toward a healthier, more confident smile—contact us today and experience the difference personalized dental care can make.