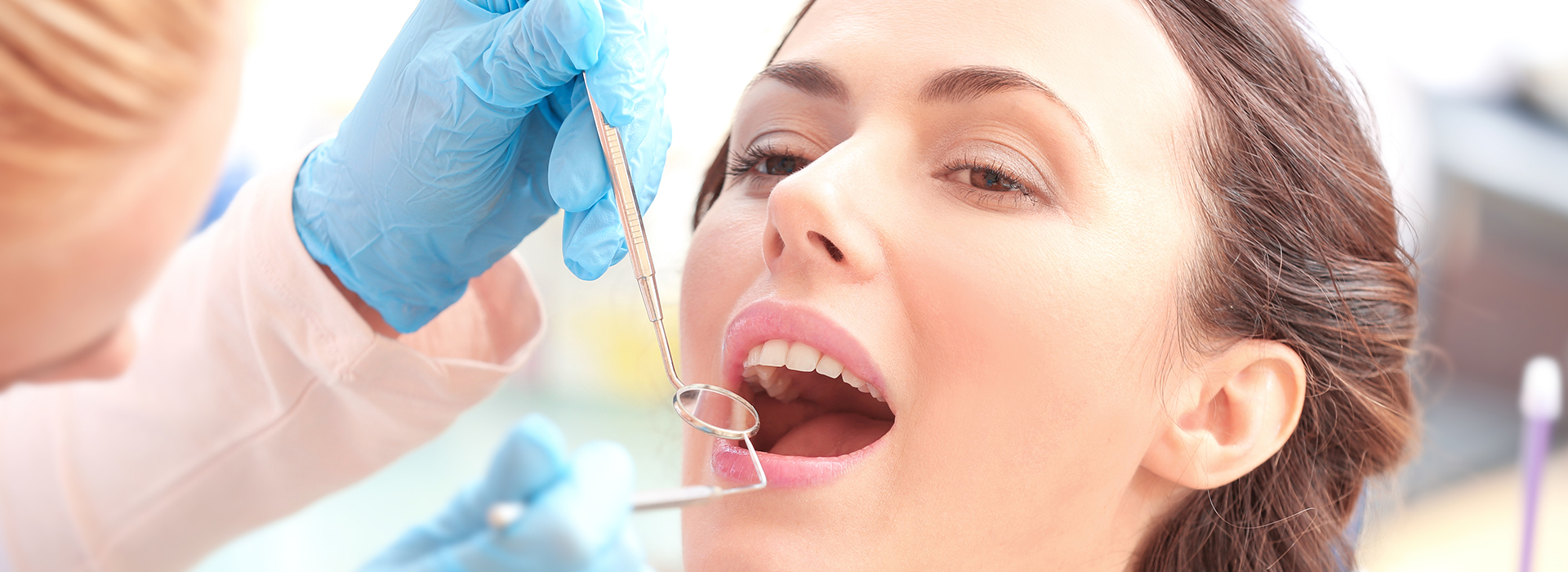
Gum disease is the leading cause of tooth loss for adults, and it affects far more people than most realize. The Centers for Disease Control and Prevention estimate that roughly half of adults over 30 show signs of periodontal disease. The condition is driven by bacteria in plaque and calculus, but the encouraging reality is that early detection and good oral care make periodontal problems largely preventable. At the office of Comprehensive Family Dentistry, we focus on clear information and practical treatment plans to protect your gums and preserve your smile.
Periodontal disease is an umbrella term for inflammatory conditions that affect the periodontium — the gums, ligaments, and bone that support your teeth. It begins when bacteria collect along the gumline and trigger an immune response. Left unchecked, that response can damage the tissues that keep teeth stable.
Because early-stage gum disease is often painless, many people don’t notice it right away. That’s why routine dental exams and professional cleanings are so important: they give clinicians the chance to spot subtle changes before those changes become irreversible.
Pay attention to persistent changes in your mouth. The following list highlights common warning signs that warrant evaluation by a dental professional:
Gums that look swollen, tender, or distinctly red
Bleeding during brushing or flossing, even when gentle
Receding gumlines or exposed root surfaces that make teeth appear longer
Increased sensitivity to hot, cold, or sweet foods and drinks
Persistent bad breath or a lingering metallic taste
Teeth that feel loose, shift, or develop new spacing
Changes in the fit of partial dentures or unexpected discomfort with a bite
Any pus, discharge, or unusual drainage around the gums
New or ongoing pain when chewing or biting down

Healthy gums do more than preserve your smile — they help maintain overall health. Research continues to show links between periodontal inflammation and systemic conditions such as cardiovascular disease, diabetes control, and certain respiratory illnesses. While the exact relationships are complex, keeping inflammation under control in the mouth contributes favorably to whole-body health.
Prevention and early intervention are cornerstones of modern periodontal care. Our team emphasizes routine screening, patient education, and targeted treatment to stop disease before it undermines teeth or contributes to broader health risks. Simple steps taken consistently at home and in the dental office can make a significant difference.
If you’re concerned about how gum disease might affect your general health, our practice can help you understand your individual risk factors and build a plan to manage them through improved oral hygiene and regular periodontal maintenance.
Gingivitis is the earliest, reversible form of gum disease. It shows up as redness, swelling, and occasional bleeding around the gums. Because there is no permanent loss of bone or connective tissue at this stage, prompt attention usually restores the tissues to health.
Treatment for gingivitis typically focuses on removing the bacterial buildup that provokes inflammation and improving daily home care. Professional cleanings combined with a consistent brushing and flossing routine, and sometimes an antimicrobial rinse, are often enough to reverse symptoms and prevent progression.
Addressing gingivitis promptly not only protects your teeth but also reduces the chance of more intensive treatments later on. Regular checkups are the best way to ensure that early inflammation is recognized and managed effectively.

When gingivitis is not resolved, it can progress to periodontitis, a stage where the supporting bone and connective tissues begin to break down. This process creates periodontal pockets — deeper spaces between the tooth root and gum — that harbor bacteria and accelerate damage. Over time, untreated periodontitis can lead to tooth mobility and tooth loss.
Periodontitis is described in degrees (mild, moderate, severe) based on pocket depth, bone loss, and tissue attachment levels. Each case is unique, so treatment plans focus on halting disease activity first, then rebuilding or stabilizing the supporting structures as much as possible.
Early detection of periodontitis improves the prospects for successful management. Even when some tissue has been lost, modern techniques aim to control infection, preserve remaining structures, and, in selected cases, regenerate tissue to restore form and function.
The primary objective of periodontal treatment is to control infection and inflammation so your mouth can return to a healthy, maintainable state. Care is individualized: a comprehensive exam directs whether conservative therapies will suffice or whether surgical intervention is needed to fully address the disease.
Advances in dentistry offer a spectrum of options — from meticulous deep cleanings to targeted antimicrobials, minimally invasive laser procedures, and regenerative grafting techniques. These approaches aim to eliminate pathogenic bacteria, reduce pocket depths, and, where possible, restore lost bone and connective tissue.
Our office combines clinical assessment, modern diagnostics, and patient-centered guidance to recommend the treatments most likely to deliver lasting periodontal health. A partnership between clinician and patient — with clear instructions for daily care and routine maintenance — is essential for long-term success.
Treatment for gum disease follows a stepwise model that begins with conservative measures and progresses to more advanced procedures only if necessary. The choice of therapy depends on the severity of disease, the depth of periodontal pockets, bone levels, and the patient’s overall health and preferences.
Initial care often involves scaling and root planing, improved oral hygiene practices, and close monitoring. When the disease has caused deeper pockets or significant bone loss, surgical procedures can allow direct access to infected areas, reshape damaged tissues, and place regenerative materials when appropriate.
Regardless of the approach, the long-term outcome depends on ongoing maintenance. Periodontal therapy is most effective when combined with regular professional care and consistent home hygiene to prevent re-infection and preserve treatment gains.
When periodontal problems are detected early, conservative care can restore health without surgery. This typically involves deep cleanings that remove plaque and hardened deposits from below the gumline, smoothing the tooth roots so the gum can reattach more effectively.
Adjunctive therapies — such as localized antimicrobials placed beneath the gumline or carefully selected systemic medications — can support healing by reducing the bacterial population responsible for inflammation.
These less invasive strategies follow the dental community’s preference for the simplest effective treatments. If symptoms resolve and pocket depths become manageable, ongoing maintenance can keep the condition under control.
When pockets are too deep for non-surgical cleaning or when there is significant bone loss, periodontal surgery may be recommended to remove infection and repair damaged tissues. Surgical access allows thorough cleaning of root surfaces and reshaping of bone and gum contours.
Grafting procedures — using bone- or tissue-derived materials — and guided tissue regeneration can help rebuild lost structure and improve both function and esthetics in suitable cases. In select situations, laser technology can complement or replace conventional surgical techniques to reduce pocket depth and treat affected tissues.
The overarching goals of these procedures are to eliminate infection, preserve remaining bone, and make the dentition easier to keep clean, thereby lowering the risk of future recurrence.
Remove bacteria and infected debris from beneath the gums and from the tooth roots
Stop further destruction of bone and reshape hard tissues where appropriate
Reduce pocket depths to enable better home care and long-term maintenance
Keeping your gums healthy is one of the most important investments you can make in your overall dental well-being. If you have signs of inflammation or are due for a periodontal check, please contact us to learn more about assessment and treatment options. Our team is available to answer questions and help you choose the best path to lasting periodontal health.

Gum disease often starts with subtle symptoms that many patients overlook. Early warning signs include gums that are red, swollen, or bleed during brushing and flossing, increased tooth sensitivity, and persistent bad breath. Noticing these changes early makes it much easier to reverse inflammation and protect supporting tissues.
Because early-stage disease can be painless, routine dental exams and professional cleanings are essential for detection. During a checkup clinicians look for bleeding on probing, pocket depth changes, and any recession that might indicate disease activity. Prompt follow-up after finding these signs improves the likelihood of successful, conservative treatment.
Gingivitis is the earliest, reversible form of gum disease characterized by inflammation of the gum tissue without permanent loss of bone or connective tissue. Typical signs include redness, swelling, and occasional bleeding, and treatment usually involves professional cleaning and improved home care. When addressed promptly, gingivitis can be resolved and progression stopped.
Periodontitis occurs when inflammation advances and the supporting bone and ligament begin to break down, creating deeper periodontal pockets that harbor bacteria. This stage is measured by pocket depth, attachment loss, and radiographic bone changes and may require more extensive therapy to halt progression. While some tissue loss can be managed or partially regenerated with modern techniques, long-term control depends on effective treatment and maintenance.
Diagnosis begins with a comprehensive clinical exam that includes measuring pocket depths around each tooth, checking for bleeding on probing, assessing tooth mobility, and evaluating gum recession. X-rays are used as needed to assess bone levels and reveal changes that are not visible on the surface. Your clinician will also review medical history and risk factors such as smoking, diabetes, and medications that can affect periodontal health.
At Comprehensive Family Dentistry, findings from the exam and imaging are combined to classify the condition and guide treatment decisions. A personalized plan is then developed to address active infection, stabilize supporting structures, and set a schedule for re-evaluation. Regular monitoring allows the team to track response to therapy and adjust care if disease activity continues.
Conservative treatment typically starts with scaling and root planing, a deep cleaning that removes plaque and hardened deposits from below the gumline and smooths root surfaces to encourage reattachment. Adjunctive therapies may include localized antimicrobials placed beneath the gumline, medicated rinses, or a short course of systemic medication in selected cases. Patient education and improved daily oral hygiene are fundamental parts of this phase.
After initial therapy, clinicians reassess pocket depths and inflammation to determine whether additional treatment is needed. When non-surgical care reduces pocket depths to a maintainable level, periodontal maintenance visits are scheduled at regular intervals to prevent recurrence. This stepwise approach favors the least invasive effective therapies first and reserves advanced procedures for cases that require them.
Surgical intervention is considered when pockets remain too deep for effective non-surgical cleaning or when there is significant bone loss that impairs support for the teeth. Surgery provides direct access to thoroughly remove infection, reshape damaged bone and soft tissues, and create an anatomy that is easier to keep clean. The decision to proceed with surgery depends on pocket depth, bone levels, patient health, and treatment goals.
Regenerative techniques such as bone grafting and guided tissue regeneration may be recommended in cases where restoring lost structure can improve function and prognosis. These procedures aim to rebuild bone and connective tissue in suitable sites, improving stability and long-term outcomes. The treatment plan always balances potential benefits, patient preferences, and realistic expectations for healing and maintenance.
Laser therapy can be used as an adjunct to traditional periodontal treatment to reduce bacterial load, remove diseased pocket lining, and encourage tissue healing with minimal invasiveness. While lasers may complement scaling and root planing or certain surgical procedures, they are typically part of a combined approach rather than a standalone cure. The choice to use laser therapy depends on individual clinical findings and evidence-based assessment.
Antimicrobial therapies, including localized antibiotic delivery and therapeutic mouth rinses, support mechanical cleaning by targeting bacteria that drive inflammation. Systemic antibiotics are reserved for specific aggressive or refractory cases where topical measures are insufficient. Your clinician will select adjunctive options based on the severity of disease, microbial profile, and the overall treatment plan.
Daily home care is a cornerstone of periodontal health and includes thorough toothbrushing at least twice a day and cleaning between teeth with floss or interdental brushes once daily. Using an antimicrobial or fluoride rinse as recommended and replacing a toothbrush every three months or sooner helps maintain a clean oral environment. Consistent, gentle technique is more effective than aggressive brushing that can harm gums.
Lifestyle factors also influence healing and disease control; quitting tobacco, managing blood sugar if you have diabetes, and maintaining a balanced diet support oral and overall health. Attend scheduled periodontal maintenance visits so your dental team can monitor pocket depths and reinforce home care instructions. Good communication with your clinician about medications and medical changes helps tailor care to your needs.
Research shows associations between periodontal inflammation and systemic conditions such as cardiovascular disease, poorer diabetes control, and certain respiratory issues, likely linked through chronic inflammation and bacterial exposure. While these relationships are complex and still under study, controlling oral inflammation is considered part of a holistic approach to health. Maintaining periodontal health can therefore contribute favorably to general well-being.
Your dental team will review your medical history and work with you and your physicians when needed to manage shared risk factors. Addressing gum disease proactively can reduce inflammatory burden and support better outcomes for other chronic conditions. Clear communication about health status and coordinated care help ensure safe and effective periodontal treatment.
Referral to a periodontist is appropriate when periodontal disease is advanced, when pocket depths and bone loss are beyond what can be managed predictably with conservative care, or when specialized surgical or regenerative procedures are indicated. Patients with complex medical conditions, recurrent disease despite therapy, or cases requiring implant placement in compromised sites also benefit from specialist expertise. Referrals ensure patients have access to the full range of treatment options when needed.
General dentists and periodontists often collaborate to provide coordinated care tailored to the patient’s goals and health needs. A referral does not mean primary care is being abandoned; it is a partnership to achieve the best long-term outcome. Your clinician will discuss the reasons for referral and help you understand what to expect from specialist evaluation and treatment.
Your initial periodontal appointment typically includes a full clinical assessment, periodontal probing, and any necessary imaging to evaluate bone levels and identify areas of active disease. Conservative treatment such as scaling and root planing is often the first step and may be performed under local anesthesia for comfort, followed by a scheduled re-evaluation to measure healing. If deeper treatment is required, the team will explain surgical or regenerative options and the anticipated recovery process.
After active therapy you will be placed on a periodontal maintenance schedule with visits tailored to your risk profile to monitor pocket depths and prevent recurrence. Our Miami Lakes team emphasizes patient education, practical home care strategies, and clear follow-up so you understand each stage of treatment. The goal is to restore and maintain a healthy, stable periodontium while minimizing the need for future invasive care.

Whether you’re ready to schedule your next dental appointment or simply have questions about our services, connecting with our team has never been easier.
Our friendly team is here to assist with appointment scheduling, answer questions about treatments, and address any concerns you may have. You can call or use our convenient online form to get in touch.
Take the first step toward a healthier, more confident smile—contact us today and experience the difference personalized dental care can make.