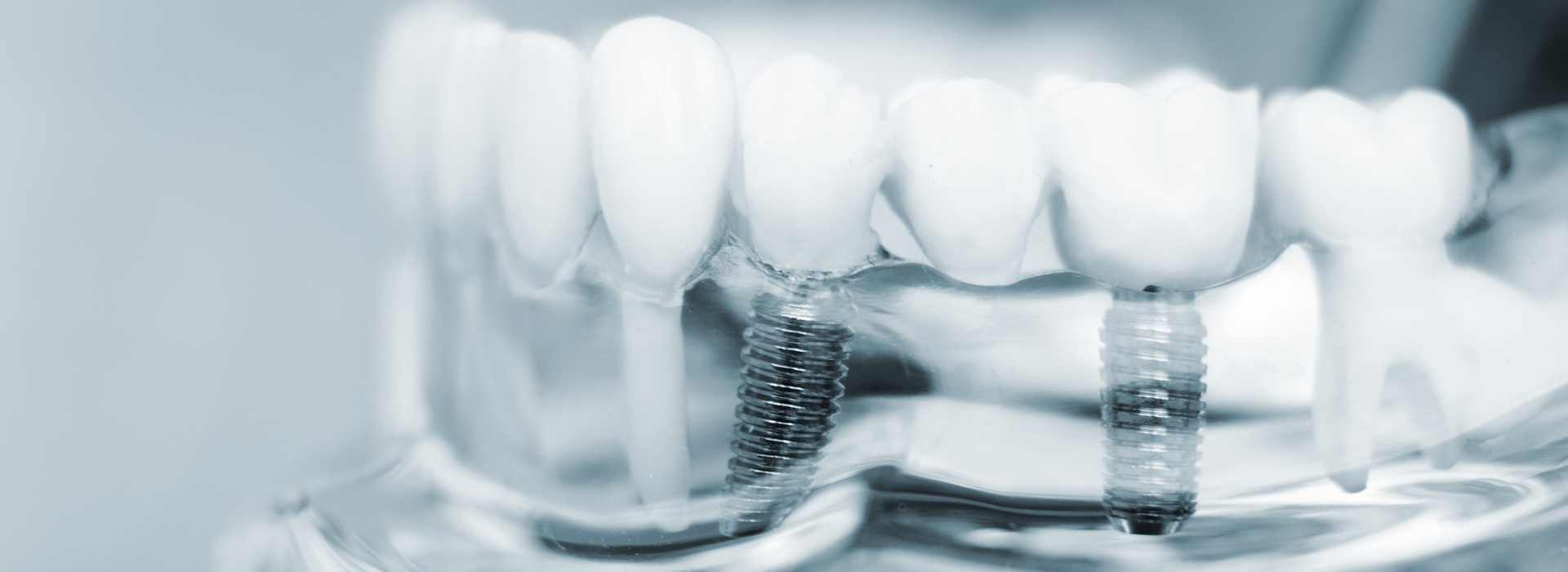
Tooth loss affects millions of Americans and can change how you eat, speak, and carry yourself in everyday life. Whether the cause is decay, gum disease, or an injury, replacing missing teeth restores more than appearance — it preserves oral function and long-term jaw health. Modern implant dentistry is designed to rebuild a stable, natural-feeling bite while protecting the structures that support your face and smile.
Dental implants are engineered to act like the root of a natural tooth. When placed and allowed to bond with the jawbone, they become a durable foundation for crowns, bridges, or removable prostheses. This root-level approach preserves bone, supports facial contours, and avoids the common downsides of traditional tooth replacement methods that rely on neighboring teeth for support.

At Comprehensive Family Dentistry, we emphasize treatments that restore both appearance and lasting oral health. For many patients, implants offer a return to everyday pleasures — eating hearty foods, speaking without worry, and smiling confidently — with results that are both predictable and long lasting.
An implant consists of a biocompatible post, typically made of titanium or a titanium alloy, that is surgically placed into the jawbone. Over the subsequent months it integrates with the surrounding bone in a process called osseointegration, creating a strong anchor similar to a tooth root. Once integration is secure, a precisely crafted crown or prosthesis is attached to restore chewing function and aesthetics.
This root-like stability is what sets implants apart: they transmit biting forces into the bone, which helps preserve bone volume and prevents the ridge shrinkage that commonly follows tooth loss. Because implants operate independently of adjacent teeth, they usually avoid the need to alter neighboring healthy teeth for support.
For patients who want a natural look and feel without compromising nearby teeth, implants are a restorative option that balances long-term function with conservative dental care.
Dental implants remove many of the practical limitations associated with removable dentures. Eating becomes easier and more comfortable because implants lock restorations in place and allow patients to chew with confidence. Speech is often clearer when teeth are stable and properly positioned, and the worry of slippage or adhesive dependence is greatly reduced.
Maintenance is also straightforward: implants are cared for much like natural teeth, with thorough brushing, flossing, and routine dental exams. While implants themselves cannot decay, the soft tissues and adjacent teeth still require protection and professional monitoring to ensure the best long-term results.
These practical advantages make implants a compelling option for adults seeking a durable, low-maintenance solution to missing teeth.
Implant dentistry is flexible by design. Treatment can be customized to replace a single missing tooth, several teeth, or an entire dental arch. During an exam, your dentist evaluates bone volume, gum health, bite mechanics, and cosmetic goals to design the approach that best suits your needs and lifestyle.
Because every smile is unique, the restorative plan may combine implants with crowns, bridges, or specially designed implant-retained dentures to achieve the optimal balance of function and appearance. The goal is always a solution that feels natural, looks harmonious with your face, and stands the test of time.
When one tooth is missing, a single implant restored with a crown replaces it without affecting adjacent teeth. This approach conserves natural tooth structure because it eliminates the need to prepare neighboring teeth for a traditional fixed bridge. The result is a self-supporting restoration that closely mimics the form and function of the original tooth.
Single-tooth implants are often the most conservative long-term choice for isolated tooth loss because they preserve bone and maintain healthy spacing in the mouth.
Successful implant care begins with thorough planning. Diagnostic imaging, a review of medical and dental history, and precise measurement of the jawbone guide the team in selecting implant size, angle, and restorative design. Planning may also include digital models and surgical guides to increase accuracy and predictability.
Placement is typically an outpatient procedure performed under local anesthesia, with sedation available for anxious patients. The surgical phase is followed by a healing period in which the implant fuses to the bone. Depending on the case, a temporary restoration can be placed to maintain appearance and basic function during healing.
During implant placement, careful tissue management and precise positioning protect surrounding teeth and nerves. Most patients experience manageable post-operative discomfort that subsides within a few days, and follow-up visits allow the clinician to monitor healing and address any concerns. Clear pre- and post-operative instructions help minimize complications and support steady recovery.
Osseointegration typically takes several months. Once the implant is firmly integrated, the restorative team fabricates the final crown, bridge, or denture to ensure a natural appearance and accurate bite. Communication between surgical and restorative phases is key to achieving a seamless outcome.
After restoration, regular dental checkups are essential to monitor tissue health, confirm the stability of the restoration, and maintain hygiene. Professional cleanings and patient diligence in oral hygiene reduce the risk of complications such as peri-implant inflammation. With proper care, implants present a predictable solution for durable tooth replacement.
A reliable bone foundation is critical to implant success. Where bone volume has diminished due to long-term tooth loss, periodontal disease, or trauma, grafting procedures can rebuild lost height and width to provide a secure site for implant placement. These techniques make implants possible for patients who might otherwise be poor candidates.
Bone grafting can be performed at the time of extraction, before implant placement, or simultaneously with implant surgery, depending on the clinical situation. Materials and methods vary, but the common goal is to create stable bone that will integrate reliably with the implant.
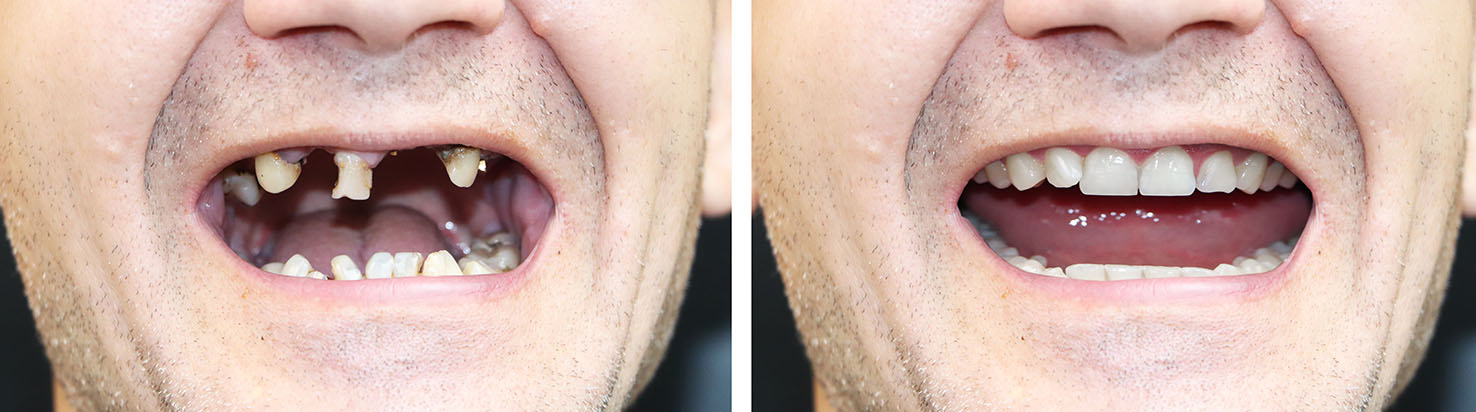
Grafting is considered when imaging reveals insufficient bone to securely support an implant. In some cases a sinus lift or ridge augmentation is recommended to raise or widen the supporting bone. These procedures are well documented and, when paired with careful planning, can produce predictable results that enable successful implant placement.
Modern biomaterials, membrane techniques, and gentle surgical protocols shorten healing times and improve outcomes. Your dentist will explain the options and the anticipated timeline so you can make an informed decision about preparatory care.
Advanced imaging like cone-beam CT provides three-dimensional views of the jaw, helping clinicians assess bone volume, nerve positions, and anatomic landmarks with precision. When combined with digital planning and surgical guides, this technology improves implant placement accuracy and reduces surgical surprises, contributing to higher success rates and smoother recoveries.
Implants are designed for longevity, but their success depends on thoughtful maintenance and routine professional care. Good oral hygiene, regular dental visits, and attention to gum health are crucial to preventing inflammation around the implant and to preserving surrounding bone and tissue.
Compared with alternative restorations, implants often provide superior function and stability. They help maintain facial structure by preserving bone and avoid the collateral damage to adjacent teeth that some traditional options can cause. For many patients, implants represent an investment in long-term oral health and quality of life.
Not every patient will follow the same treatment path, but most adults with reasonably healthy gums and sufficient bone are candidates for implants. During a consultation, your provider will review your medical history, examine your mouth, and outline a personalized treatment plan that reflects your goals and health needs.
If supplemental treatments such as grafting or periodontal therapy are recommended, your dentist will explain why they matter and how they contribute to predictable implant success. The decision to move forward is made together, with a focus on achieving a durable, natural-feeling result.
Dental implants restore more than teeth: they restore function, facial support, and the confidence to enjoy everyday life without compromise. Implant therapy combines surgical precision, restorative craftsmanship, and ongoing preventive care to deliver results that last. Comprehensive Family Dentistry brings focused experience and modern planning tools to help patients decide whether implants are the right solution for their smile.
If you’d like to explore implant options or learn more about what to expect from treatment, please contact us for more information.

Dental implants are medical-grade posts that replace the root portion of a missing tooth and provide a stable foundation for a crown, bridge or denture. The implant is typically made of titanium or a biocompatible alloy and is placed into the jawbone where it integrates through a process called osseointegration. Once integration is complete, the implant supports a restoration that restores chewing function and a natural appearance.
Because implants transmit bite forces into the bone like a natural tooth root, they help preserve jawbone volume and facial contours that can diminish after tooth loss. Implants function independently of adjacent teeth, so healthy neighboring teeth usually do not need to be altered. This root-level approach is why implants are often considered the most durable restorative option for replacing missing teeth.
Many adults with one or more missing teeth can be candidates for dental implants, provided they have healthy gum tissue and adequate jawbone to support the implant. Patients with reduced bone volume may still qualify after preparatory procedures such as bone grafting or a sinus lift, and a thorough clinical evaluation and imaging study will determine suitability. The treatment plan also considers overall health, medications and lifestyle factors that could affect healing.
Certain medical conditions or habits, such as uncontrolled diabetes or heavy smoking, can increase risks and may require additional management before implants are placed. Your dentist will review your medical history, assess oral health and discuss any modifications needed to optimize outcomes. A personalized consultation ensures the proposed approach matches your health profile and long-term goals.
Dental implants provide root-level support that preserves bone and delivers strength and stability similar to natural teeth, which often results in improved chewing efficiency and comfort. Traditional bridges rely on adjacent teeth for support and require preparation of those teeth, while removable dentures sit on the gums and can shift or require adhesives. Because implants function independently, they typically avoid the collateral wear or structural compromise that some fixed bridges can cause.
Implant-supported restorations can be used to replace a single tooth, several teeth or an entire arch, offering flexibility in restorative options. Removable implant-retained dentures offer improved retention compared with conventional dentures while fixed implant bridges can restore a full arch without relying on nearby teeth. The choice among these options depends on oral health, bone volume and the patient’s functional and aesthetic priorities.
Treatment begins with a comprehensive exam that often includes three-dimensional imaging such as cone-beam CT to evaluate bone volume, nerve anatomy and sinus position, allowing precise treatment planning. The surgical stage places the implant into the jawbone under local anesthesia, and the implant is allowed to integrate with the bone over several months while a temporary restoration may be used to maintain appearance and function. After osseointegration is confirmed, the restorative phase attaches a custom crown, bridge or denture to achieve the final form and bite.
Throughout the process the care team coordinates surgical planning and prosthetic design to ensure accurate positioning and a natural-looking outcome. Surgical guides and digital planning tools increase predictability and help reduce surprises during surgery. At Comprehensive Family Dentistry we emphasize detailed planning and clear communication between surgical and restorative phases to deliver predictable, long-lasting results.
Most implant placements are performed with local anesthesia to numb the surgical area, and many patients report minimal discomfort during the procedure. For patients with dental anxiety or for more complex cases, additional sedation options such as oral sedatives or nitrous oxide may be offered to promote relaxation and comfort. After surgery, a short period of soreness, swelling and mild discomfort is common and is typically managed with prescribed or over-the-counter medications and cold compresses.
Your dentist will provide clear pre- and post-operative instructions to minimize pain and support healing, including dietary recommendations and oral hygiene guidance. Follow-up visits allow the clinician to monitor healing and address any concerns promptly. Communicating any unexpected pain, prolonged swelling or numbness ensures complications are identified and treated quickly.
When placed and maintained properly, dental implants are designed to last for many years and often for a lifetime, while the prosthetic components such as crowns or denture teeth may require replacement over time. Long-term success depends on good oral hygiene, regular professional care and control of risk factors such as smoking, untreated periodontal disease and bruxism (teeth grinding). The choice of implant materials and the precision of the surgical and restorative work also influence durability.
Routine dental checkups let your dentist evaluate implant stability, surrounding tissue health and prosthetic wear so issues can be addressed early. Protective habits such as wearing a night guard if you grind your teeth and avoiding hard impacts on restorations support longevity. With attentive maintenance, implants offer a predictable and resilient solution for tooth replacement.
Bone grafting is a surgical technique used to rebuild lost jawbone so it can support an implant reliably, and it is commonly recommended when bone volume has decreased after tooth loss, periodontal disease or trauma. Grafting material may be sourced from the patient, a donor source or synthetic biomaterials, and the procedure can restore height or width of the ridge or lift the sinus floor for upper posterior implants. In many cases bone can be augmented at the time of extraction or staged before implant placement depending on clinical needs.
Modern grafting methods and gentle surgical protocols improve predictability and often shorten healing times, but grafting does add steps and a healing interval to the overall treatment timeline. Your dentist will explain the rationale for grafting, the expected healing progression and how it contributes to reliable implant integration. Careful imaging and planning help determine whether grafting is needed and which technique best fits a patient’s anatomy.
Home care for implants emphasizes the same core practices as natural teeth: thorough brushing twice daily with a nonabrasive toothbrush and daily interdental cleaning using floss, floss threaders or interdental brushes designed for implants. Effective plaque removal at the gumline and between teeth is essential to prevent peri-implant inflammation and protect the supporting bone. Avoiding tobacco and managing medical conditions that affect healing also supports long-term implant health.
Regular professional cleanings and periodontal assessments are important because hygienists use instruments and techniques designed to clean around implant restorations safely. Your dental team will tailor a maintenance schedule and demonstrate the most effective tools and methods for your specific restoration. Promptly reporting any bleeding, swelling or looseness helps the clinician intervene early and preserve the implant site.
Although implant success rates are high, potential complications include infection around the implant (peri-implantitis), insufficient integration, nerve irritation in rare cases and sinus complications for upper posterior placements. Many of these risks are reduced by careful planning with three-dimensional imaging, precise surgical technique and control of risk factors such as smoking and untreated gum disease. Early signs of a problem often include persistent inflammation, bleeding or discomfort, and timely evaluation improves the chance of a favorable outcome.
Your dentist will discuss individualized risks during the consultation and recommend steps to minimize them, such as infection control, staged treatment when necessary and close follow-up care. Good communication about medical history, medications and healing concerns is essential for safe treatment. With appropriate planning and maintenance, most complications are uncommon and manageable.
To begin, schedule a consultation so the dentist can review your medical and dental history, perform an oral exam and obtain diagnostic imaging to evaluate bone volume and anatomic considerations. During the visit you will discuss restorative goals, the recommended timeline and any preparatory treatments such as grafting or periodontal care that would improve predictability. The consultation is an opportunity to ask about anesthesia options, expected healing and the sequence of surgical and restorative visits.
Our approach emphasizes personalized planning and clear communication so patients understand each step and the rationale behind recommended treatments. Treatment decisions are made collaboratively to align clinical needs with patient expectations and lifestyle. If you decide to proceed, the team will outline the plan, prepare a realistic timeline and coordinate surgical and prosthetic phases to support a smooth experience.

Whether you’re ready to schedule your next dental appointment or simply have questions about our services, connecting with our team has never been easier.
Our friendly team is here to assist with appointment scheduling, answer questions about treatments, and address any concerns you may have. You can call or use our convenient online form to get in touch.
Take the first step toward a healthier, more confident smile—contact us today and experience the difference personalized dental care can make.