
Deciding to remove a tooth is never taken lightly. In many cases we can repair or preserve a tooth, but there are situations where extraction is the most predictable way to protect the rest of your mouth. Our approach is to weigh short-term disruption against long-term oral health so patients and their families can make informed choices.
Before recommending extraction, we review the medical and dental history, current symptoms, and the likely outcomes of alternative treatments. This helps ensure any recommendation supports overall health, function, and future restorative possibilities. We also discuss options for replacing a missing tooth when appropriate, so patients understand the sequence of care.
Comfort and safety guide every step. We explain how we control pain and anxiety, what to expect during the visit, and how recovery usually progresses. Clear communication helps reduce worry, and careful planning reduces complications so you can return to normal activities as quickly as possible.
There are several predictable patterns that make extraction the most appropriate clinical decision. Some start early in childhood, such as retained baby teeth that interfere with proper eruption. Others develop later in life because of trauma, infection, or progressive disease that leaves a tooth beyond repair.
We use examination and imaging to determine whether a tooth is restorable. When the damage extends into the tooth’s core, when the supporting bone is severely compromised, or when a tooth endangers nearby structures, extraction becomes a responsible option to prevent further problems and to preserve overall oral function.
Below are the typical conditions that may prompt a recommendation for extraction. Each entry explains why removal can be better for health and how we evaluate the situation carefully before moving forward.
Baby teeth that don't make way for permanent teeth
Sometimes a primary tooth remains firmly in place after its permanent successor is ready to erupt. When a baby tooth’s roots fail to resorb or the tooth becomes fused to the bone, it can block normal development and alignment. Removing that tooth at the right time can prevent crowding and guide the permanent tooth into its proper position.
Severe decay that leaves a tooth non-restorable
Decay begins at the enamel and, if untreated, advances toward the inner structures of the tooth. Once so much structure is lost that a reliable restoration is no longer possible, extraction removes the source of infection and pain. Doing so protects adjacent teeth and the supporting bone from further damage.
Teeth fractured beyond repair
Trauma and large fractures can leave insufficient tooth structure for crowns or other repairs. If a break extends below the gumline or involves the root in a way that compromises long-term stability, extraction may be the healthiest option to avoid recurrent problems or persistent infection.
Advanced periodontal disease
When gum disease has significantly reduced the bone and soft tissue supporting a tooth, that tooth may loosen and become a chronic source of infection. In advanced cases, removing the affected tooth can reduce inflammation, improve oral health, and make it easier to restore chewing function with prosthetic options later.
Problematic wisdom teeth
Third molars often lack adequate space to erupt normally. Impacted or partially erupted wisdom teeth can trap food and bacteria, damage adjacent teeth, or contribute to cyst formation. Early assessment helps determine whether removal now will prevent complications down the road.
Teeth extracted as part of orthodontic planning
In some orthodontic cases, selective removal of permanent teeth provides space to align the remaining teeth in a healthier, more stable bite. This decision is made in collaboration with your orthodontist, with the long-term goal of improving function and aesthetics.
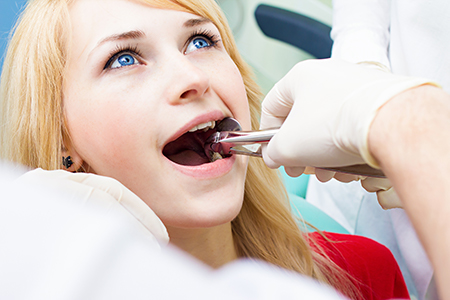
Preparation begins with a thorough review of your medical and dental records, current medications, and any health conditions that could affect treatment. Accurate information about heart conditions, joint replacements, or medications that affect bleeding helps us plan safely and coordinate with your physician if needed.
We typically capture digital radiographs to evaluate root anatomy, bone levels, and the relationship of the tooth to nearby structures. Imaging allows us to determine whether a straightforward removal is likely or if a surgical approach may be required. We will explain our findings and recommend the most predictable path forward.
Comfort is a priority: local anesthesia reliably numbs the area, and for patients with anxiety or complex needs we discuss sedation options to ensure a calm, safe experience. We will also review pre-operative instructions—such as medication guidance or fasting recommendations—so you arrive prepared for the procedure.
On the day of the extraction, your team will review the plan, answer questions, and ensure you’re comfortable before beginning. Our goal is to provide care that minimizes discomfort, limits procedure time when possible, and protects oral health for the long term.
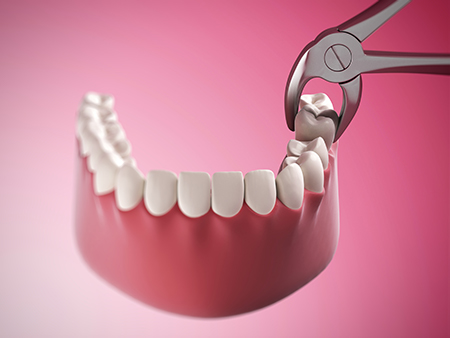
Not every extraction is the same. Some teeth can be removed with forceps after the tissues are numbed—these are generally quicker and heal more predictably. Other teeth, such as those that are broken at the gumline, fused to bone, or impacted, require a surgical approach that provides access and control to remove the tooth safely.
A simple extraction is indicated when a tooth is fully visible and the roots are accessible without removing bone. After anesthetizing the area, the tooth is gently loosened and lifted with instruments designed for atraumatic removal. This technique preserves surrounding bone and soft tissue when possible and supports more predictable healing.
Patients who are nervous about the procedure can discuss additional comfort options, including oral or intravenous sedation, which help manage anxiety while maintaining safety and monitoring.
Surgical extractions are used for teeth that cannot be removed intact with forceps—this may involve removing small amounts of bone, creating a small incision, or sectioning the tooth into pieces so it can be removed with minimal trauma. Complex cases are sometimes referred to an oral and maxillofacial surgeon when advanced techniques or sedation are needed.
Regardless of complexity, we plan each surgical extraction to minimize inflammation, protect adjacent teeth and nerves, and provide clear post-operative instructions to support healing.
Recovery after an extraction varies by the procedure’s complexity and the individual patient. Generally, the first 24–48 hours are the most critical for clot formation and the beginning of tissue repair. Following straightforward precautions dramatically reduces the risk of complications and helps the site heal comfortably.
We supply specific post-operative instructions tailored to your case, including guidance on activity limitations, medications, and oral care. If sutures were placed or additional monitoring is needed, we will schedule a follow-up visit to check healing and remove stitches if required.
If unusual symptoms arise—such as persistent bleeding, increasing pain despite medication, or signs of infection—contact our office so we can evaluate the situation and intervene if necessary. Early attention prevents minor issues from becoming more significant concerns.
Apply firm but gentle pressure
You will be given gauze to maintain pressure at the extraction site to control bleeding. Replace the gauze as instructed and keep steady pressure for the initial period to encourage clot formation. Mild oozing for up to 24 hours is common, but excessive bleeding should prompt a call.
Protect numb tissues
Avoid chewing or touching the area while local anesthesia is in effect. Numb lips and tongue are easily injured, so take extra care until sensation returns fully.
Follow medication instructions
Antibiotics:
If prescribed, take the full course exactly as directed to reduce the risk of infection.
Pain control:
Start pain medication as recommended before numbness wears off for greater comfort. Use over-the-counter or prescription options according to the instructions we provide.
Avoid disturbing the clot
Do not rinse vigorously, spit, or use a straw for the first day or two. These actions can dislodge the clot and delay healing.
Control swelling
Apply an ice pack intermittently during the first 24 hours to minimize swelling. Use 10- to 15-minute on/off cycles as needed.
Refrain from tobacco
Smoking and vaping impair healing and increase the risk of complications. Avoid tobacco products for at least a week following the procedure, or as directed by your provider.
Choose gentle nutrition
In the first days after surgery, favor cool or lukewarm soft foods and avoid hot, spicy, or carbonated beverages. Keep hydrated and progress to firmer foods as comfort allows.
Maintain careful oral hygiene
Brush surrounding teeth gently and, when appropriate, rinse with a mild warm saltwater solution to keep the area clean. Follow your provider’s timeline for when to resume normal brushing and rinsing at the extraction site.
Keep scheduled follow-up visits
Return appointments let us confirm that the site is healing as expected and address any concerns promptly. If stitches were placed, they will be monitored and removed or allowed to resorb according to the type used.
If you notice ongoing bleeding, increasing pain, swelling that worsens after a few days, or any other unusual symptom, contact our office so we can assess and guide the next steps.
Comprehensive Family Dentistry approaches extractions with an emphasis on gentle technique, clear communication, and long-term planning. We focus on protecting healthy tissue, preventing complications, and discussing replacement options when a tooth removal affects function or appearance.
When an extraction is recommended, you’ll receive an individualized plan that reflects your medical history, restorative goals, and comfort needs. We coordinate care when referrals are appropriate and provide clear aftercare instructions so healing proceeds smoothly.
Our goal is to help patients move from a problem tooth to a healthy, stable solution—whether that means healing on its own, planning for a prosthetic replacement, or coordinating with specialists for more complex care.
In summary, tooth extraction is sometimes the most responsible treatment to protect mouth health. We evaluate each case carefully, use modern techniques to minimize discomfort, and support patients through recovery and follow-up. Contact us to learn more or to discuss whether extraction is the best option for your situation.

Extractions are recommended for several common reasons. These include severe decay that leaves the tooth nonrestorable, advanced periodontal disease that has destroyed supporting bone and gum tissue, and significant fractures that prevent repair. Other frequent causes are impacted or poorly positioned wisdom teeth, persistent primary teeth that block normal eruption, and crowding when orthodontic treatment requires creating space.
Your dentist will review your medical and dental history, take appropriate radiographs, and consider conservative alternatives before recommending removal. The goal of extraction is to protect your overall oral health and to prevent ongoing infection or damage to adjacent teeth and tissues. If an extraction is advised, your provider should explain the reasons and the likely next steps, including whether replacement is recommended.
A simple extraction is usually chosen when the tooth is fully visible in the mouth and the root anatomy is straightforward. In these cases the tooth is numbed with local anesthesia, loosened, and removed with forceps in a single visit. A surgical extraction is necessary when a tooth is broken below the gum line, ankylosed, impacted, or when roots are curved or fused to the jawbone.
Surgical extractions often require a small incision, removal of some bone, or sectioning the tooth to allow safe removal and may be performed by a general dentist or an oral and maxillofacial surgeon. Radiographs and a careful clinical exam guide the decision, and your dentist will discuss whether referral, additional imaging, or sedation are appropriate for your case. Preoperative planning helps reduce complications and improves healing outcomes.
Before any extraction, make sure your dental team knows your full medical history, including current medications, recent surgeries, allergies, and any chronic conditions such as diabetes or bleeding disorders. Also mention if you are pregnant, have a heart condition, or take blood thinners, as these factors can affect treatment planning and may require coordination with your physician. Honest disclosure helps the team take any necessary precautions to keep you safe.
You should also tell the dentist about prior reactions to local anesthetics or sedatives and whether you have difficulty with oral infections or cold sores. Follow any preoperative instructions your provider gives, such as fasting when sedation is planned or taking prescribed antibiotics when indicated. Notify the office if you develop a fever, a cold, or other new symptoms on the day of the appointment so your dentist can advise whether to proceed or reschedule.
On the day of an extraction, your dentist will review the treatment plan and confirm your medical history before providing local anesthesia to numb the area. For simple extractions the provider will loosen the tooth and remove it with forceps, while surgical extractions may involve a small incision and removal of bone or sectioning of the tooth. Throughout the procedure the team monitors your comfort and can offer additional sedation or pain control options for anxious patients.
After the tooth is removed, the socket may be smoothed and sutures placed if needed to promote healing. The dentist will provide clear post-operative instructions covering gauze changes, activity limits, and medications. Plan for a short recovery period and arrange for someone to drive you home if you received sedation.
Begin by maintaining firm but gentle pressure with gauze over the extraction site to help form a stable clot and reduce bleeding; change the gauze according to your dentist's instructions. Avoid rinsing vigorously, spitting, using a straw, or smoking for at least 24 to 72 hours because these actions can dislodge the clot and delay healing. Apply an ice pack intermittently to the outside of your face for the first 24 hours to manage swelling and keep your head elevated when resting.
Take prescribed or recommended pain medication as directed and complete the full course of any prescribed antibiotics. Stick to a soft, cool or lukewarm diet for the first couple of days and gradually return to normal eating as comfort allows. Begin gentle oral hygiene away from the extraction site and, after 24 hours, use a warm saltwater rinse to keep the area clean without disturbing healing tissues.
Contact your dental office promptly if you experience uncontrolled or heavy bleeding that does not improve after applying pressure, or if pain increases sharply after the first two or three days despite taking pain medication. A persistent bad taste, increasing swelling after 48 hours, fever, or drainage from the extraction site can indicate infection and should be evaluated without delay. Severe or prolonged numbness, difficulty breathing or swallowing, or any signs of an allergic reaction require immediate attention.
One specific complication to watch for is dry socket, which often causes increasing pain a few days after extraction and is commonly accompanied by an unpleasant odor or taste. If you notice these symptoms your dentist can provide targeted treatment to relieve pain and promote healing. Keeping follow-up appointments and following post-op instructions reduces the risk of complications and allows early detection when problems occur.
Wisdom teeth are typically evaluated for removal when they are impacted, partially erupted with repeated infection (pericoronitis), severely decayed, or causing damage to adjacent teeth. Extractions may also be recommended if third molars contribute to crowding, cause cyst formation, or produce chronic discomfort. Not every wisdom tooth requires removal; an individualized assessment with radiographs determines whether extraction is the best course.
Many clinicians recommend evaluating wisdom teeth in late adolescence or early adulthood because younger patients often heal more quickly and experience fewer complications. Your dentist will review the position of the teeth, the health of nearby structures, and your overall treatment goals to provide a clear recommendation. When surgical removal is necessary, the practice will explain the procedure, anesthesia options, and expected recovery.
Children may require extractions for reasons that include severely decayed primary teeth, retained baby teeth that block eruption of permanent teeth, trauma, or to support orthodontic treatment. Extractions in pediatric patients focus on preserving space and guiding normal development, and the dentist will evaluate whether a space maintainer or other follow-up treatment is needed. Decisions are made with attention to growth, behavior, and the child’s overall health.
Pediatric extractions are performed with techniques and behavior management strategies tailored to children, and sedation options are available when appropriate and safe. The dentist will provide parents with detailed pre- and post-operative instructions and coordinate care with the child's pediatrician when necessary. Comfort, clear communication, and gentle handling help make the experience as stress-free as possible for both child and family.
Whether you need to replace an extracted tooth depends on its location, function, and your overall oral health goals. Extracting a back molar may have different consequences than losing a front tooth, and your dentist will discuss the functional and aesthetic implications of the loss. In some cases no immediate replacement is necessary, while in others restoring the space prevents shifting, bite problems, and long-term issues.
Common replacement options include removable dentures, fixed dental bridges, and dental implants, each with different clinical requirements and timelines for placement. Your dentist will explain the pros and cons of each approach and coordinate any required healing period before definitive restoration. A thoughtful treatment plan helps restore chewing function, maintain facial support, and preserve the health of surrounding teeth.
Choosing a practice for extractions involves assessing clinical experience, patient comfort measures, and the availability of appropriate technology such as digital radiography for thorough evaluation. Our team emphasizes gentle, evidence-based care, clear preoperative planning, and careful post-operative follow-up to support predictable healing. We also offer sedation options and coordinate referrals when surgical expertise is required for complex cases.
At Comprehensive Family Dentistry you will receive a personalized plan that considers your medical history, long-term dental goals, and replacement options if needed. We provide clear instructions for recovery and maintain open communication so patients understand what to expect before, during, and after the procedure. If you have concerns or questions about an extraction, our team can review the evaluation and next steps with you during a consultation.

Whether you’re ready to schedule your next dental appointment or simply have questions about our services, connecting with our team has never been easier.
Our friendly team is here to assist with appointment scheduling, answer questions about treatments, and address any concerns you may have. You can call or use our convenient online form to get in touch.
Take the first step toward a healthier, more confident smile—contact us today and experience the difference personalized dental care can make.